Request a representative visit or G7 15 Day or G7 samples
Continuous glucose monitoring provides a more complete picture of a patient’s glucose levels, compared to what they’d be able to glean from a single fingerstick reading from a blood glucose meter (BGM). Greater access to more frequent glucose insights can support more effective diabetes management for you and, ultimately improving patient outcomes.

Watch a video showcasing how a continuous glucose monitoring system compares to a traditional blood glucose meter below, and keep reading to learn how the Dexcom G6 Continuous Glucose Monitoring (CGM) System can give insulin-using patients the power of glucose at a glance.
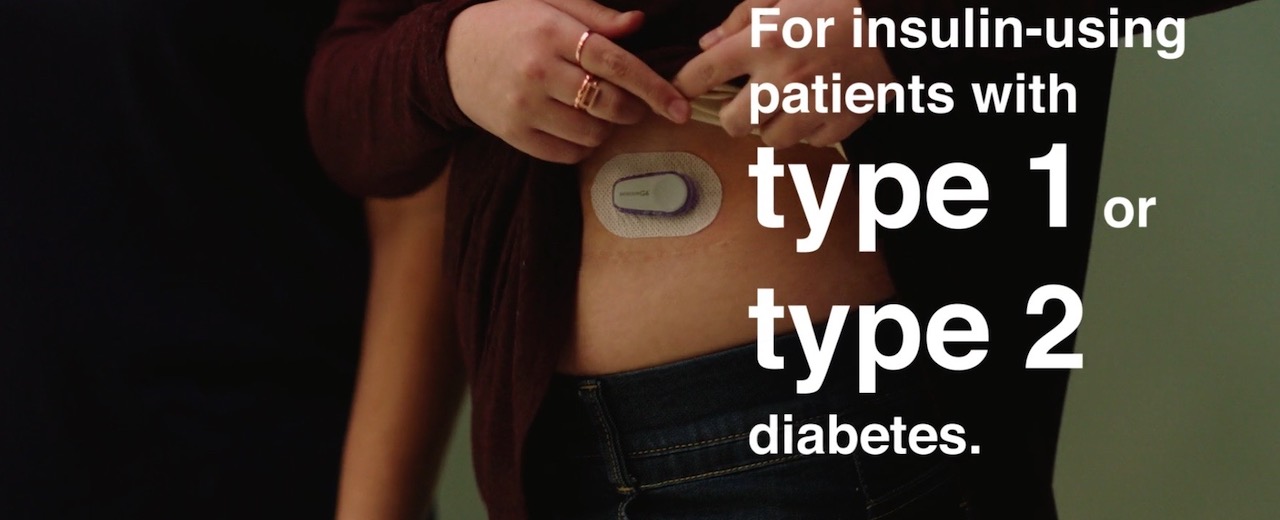

The Difference is in the Data
Patients with all types of diabetes may experience similar challenges, despite their different diagnoses. Some may struggle to understand how diet decisions affect their glucose levels, how to effectively titrate insulin, or how the timing of exercise and other activities plays a role in their treatment.
Continuous glucose monitoring technology serves to help address these issues, and more. Real-time CGM (RT-CGM) systems, like the Dexcom G6 CGM System and the all-new Dexcom G7, transmit glucose measurements at regular intervals from a wearable sensor to a nearby receiver or compatible mobile device* via Bluetooth.
Dexcom G6 and G7 CGM Systems provide users with actionable information, including historic and current glucose values and velocity of glucose change, without requiring volitional behavior.
Continuous Insight, Day and Night
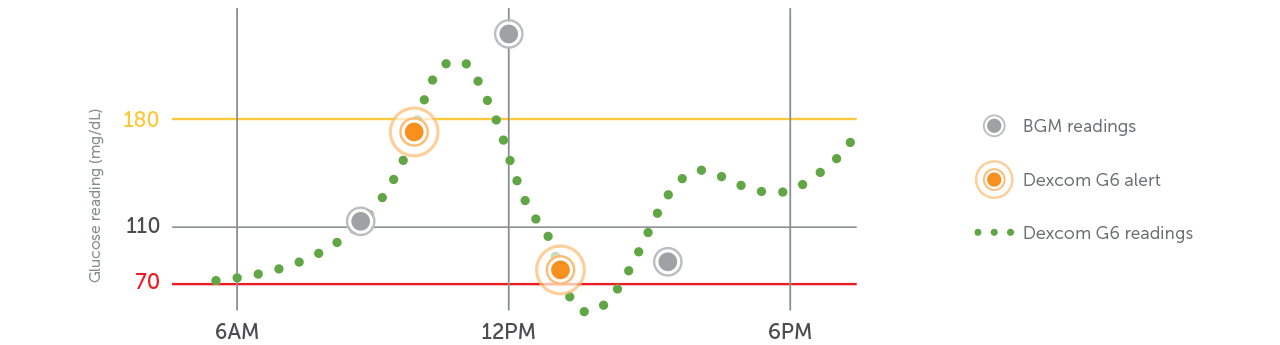
Dexcom CGM Systems helps minimize the guesswork derived from making diabetes treatment decisions based on a BGM reading alone and requires zero fingersticks† to access glucose data, helping to empower patients to self-manage their diabetes.
†If your glucose alerts and readings from Dexcom G6 or G7 do not match symptoms or expectations, use a blood glucose meter to make diabetes treatment decisions.
Primary CGM Components
The Dexcom G6 CGM System consists of four main components:

Auto-applicator
Provides simple sensor insertion at the push of a button. A patient can apply the sensor on their own by following the instructions for use.

Sensor
Monitors interstitial glucose levels through a small wire inserted just underneath the skin, sending a signal to the transmitter (10-day lifespan).

Transmitter
Fastened on top of the sensor; sends data wirelessly to the wearer's compatible display device* (3-month lifespan).

Display device
Allows patients to view their real-time glucose data and trends. Dexcom G6 also enables patients to receive a suite of alerts, an Urgent Low alarm, and other notifications on their display device,* which can help warn them of high or low glucose levels.
The Benefits of CGM for Insulin-Using Patients with T1D or T2D
Proven outcomes support your patients' progress.
Long-Term CGM Use Supports Long-Term Benefits and Outcomes
A seven year, real-world clinical trial - the longest CGM outcome study to-date - reiterates the clinical impact of using real-time CGM (RT-CGM) systems like Dexcom G6 or G7. Study participants with T1D who initiated RT-CGM within 1 year of diagnosis showed significantly reduced A1C levels compared to those who initiated RT-CGM more than three years after diagnosis or did not use RT-CGM throughout the study period.4
This supports the overarching notion that RT-CGM supports improved outcomes and diabetes management for your patients in a way that is both accessible and sustainable. Whether your patients ore sitting down for a meal, leading a presentation, or turning in for the evening, they can feel more confident in their daily diabetes treatment decisions that help shape the rest of their lives.
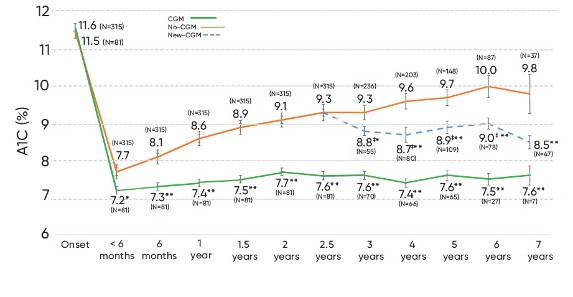
Data presented as least square mean and standard errors adjusted for age at onset, sex and insulin delivery method (insulin pump vs multiple daily injections). Number in parenthesis indicates sample size. Reduced numbers in the CGM group (and new-CGM during year 6 and 7) due to variable length of follow-up. *p<0.05, **p<0.0001 between CGM (or new-CGM) vs no-CGM group. ‡p<0.001 between new-CGM vs early CGM users.
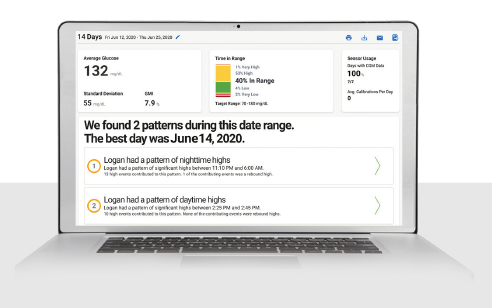
Data Sharing Options Help Connect
Care Teams
Dexcom G6 and G7 glucose data may be synced with the no-cost Dexcom Clarity software,¶ streamlining the way you can review patients’ glucose insights during in-person or telehealth appointments.
- Glucose data from your patients’ Dexcom G6 app is automatically# sent to Dexcom Clarity, removing the hassle of manual uploading.**
- Automated reports generated from the synced data offer a simplified alternative to paper logs, which can help save valuable appointment time.
- CGM interpretation using the ‘Overview’ report is billable under Medicare and private insurers (CPT code 95251).††
Dexcom CGM Systems Frequently Asked Questions
Your patient's DME distributor may be able to use the current order on-file to upgrade to Dexcom G7. The DME distributor can confirm if a new order is needed to upgrade. If a new order is needed, the distributor can fax a request to you for a Dexcom G7 order.
Your patient's current DME distributor can confirm when they are eligible to fill the next order for CGM supplies.
To determine if a smartphone is compatible with Dexcom G7, please visit https://www.dexcom.com/en-us/compatibility
-
New/Existing Pump Patients – Since it may take some time for our insulin pump partners to integrate Dexcom G7, we recommend that HCPs continue to prescribe G6 to new and existing connected pump patients until G7 is compatible with current and future automated insulin delivery systems.
-
New/Existing Patients at the Pharmacy – Dexcom G7 will be available at the pharmacy on February 17, for new and existing patients who are not using a connected insulin pump. HCPs can send their prescriptions to ASPN Pharmacies, who will coordinate fulfillment with patients at the pharmacy of their choice. For new and existing patients who are using a connected insulin pump, HCPs should continue to prescribe G6 until G7 is compatible with current and future automated insulin delivery systems.
-
New/Existing Patients at the DME Provider – Dexcom G7 will be available at Durable Medical Equipment providers on February 17th for new and existing patients who are not using a connected insulin pump. HCPs can send their prescriptions to their DME supplier, who will coordinate fulfillment with patients. For new and existing patients who are using a connected insulin pump, HCPs should continue to prescribe G6 through their DME supplier until G7 is compatible with current and future automated insulin delivery systems.
-
New Medicare Patients – You will need to provide your patients with a new prescription for G7 and work through their DME supplier to have it fulfilled. For new Medicare patients who are using a connected insulin pump, you should continue to prescribe G6 through their DME supplier until G7 is compatible with current and future automated insulin delivery systems.
-
Existing Medicare Patients – Once the patient’s G6 transmitter has expired, you will need to provide your patients with a new prescription for G7 and work through their DME supplier to have it fulfilled. For existing Medicare patients who are using a connected insulin pump and their G6 transmitter has expired, HCPs should continue to prescribe G6 through their DME supplier until G7 is compatible with current and future automated insulin delivery systems.
Because the G6 and G7 smart phone apps work independently of each other, it is possible to wear both G6 and G7 at the same time. However, if a patient wears two CGM sensors at the same time the numbers might be different because they are sensing local tissue glucose levels in separate locations on the body. Dexcom recommends using either Dexcom G6 or Dexcom G7, but not both simultaneously.
Yes, G6 will still be available to patients once G7 launches. Some patients should continue using G6 while G7 insurance coverage is expanded, and connectivity with connected insulin pumps is rolled out.
-
#1 in Accuracy1: Dexcom G7 has an overall MARD of 8.1% for pediatrics and 8.2% for adults as published in our U.S. pivotal trial data. FreeStyle Libre 3 (L3) is FDA cleared with an overall accuracy of 8.9% for adults and 9.4% for pediatrics as listed in their U.S. User Guide##.
-
Less Downtime**: G7 warms up in just 30 minutes after which you can immediately make insulin dosing decisions. L3 requires 12 hours before dosing decisions##, which would make it unable to work with a connected system in the future. Dexcom CGM Systems adherence and persistence is nearly 30% higher with Dexcom over Libre.13
-
More Reliable: G7 has an automatic predictive low alert to help prevent a low, while L3’s threshold alerts only notify you the minute after you went low##.
-
Medicare Support: RT-CGM is recommended for older adults, per ADA11 and AACE12 guidelines, and G6 and G7 both fulfill Medicare requirements. L3, Abbott’s only RT-CGM, does not fulfill Medicare requirements due to the lack of a dedicated receiver.
-
Most Proven Outcomes: Dexcom generates the most amount of clinical data and has been evaluated in a greater number of studies1 – over 300 clinical trials – on the value and benefit of CGM across the spectrum of diabetes states and methodologies to remain focused on measuring and driving the best outcomes.
-
Proven Connectivity Platform: Dexcom G7 is already part of Dexcom’s industry leading connected CGM ecosystem1 to allow patients to manage their diabetes with the insulin and lifestyle hardware and software that works best for them. With 4 years of proven connectivity and a saleable real-time API, Dexcom is the only CGM brand to offer AID and have a larger connectivity platform. L3 explicitly has an AID contraindication.##
-
Overall Patient Experience: Dexcom is the #1 most recommended CGM brand by both patients and HCPs 6, #1 in patient retention7, and #1 in patient satisfaction§§. Libre users switch to Dexcom 3x more frequently than Dexcom users switch to Libre8.
*Smart device, sold separately, required to display readings on watch. †Compatible smart devices sold separately. For a list of compatible devices, visit dexcom.com/compatibility. ||Results obtained with a prior generation Dexcom CGM System. ¶Separate Follow app and internet connection required. Users should always confirm readings on the Dexcom G6 app or receiver before making treatment decisions. #Compared to a prior generation Dexcom CGM System. **Dexcom G7 can complete warmup within 30 minutes, whereas other CGM brands require up to an hour or longer. ††Healthcare providers can register for Dexcom Clarity at clarity.dexcom.com/professional/ registration. ‡‡An internet connection is required for patients to send their glucose data to Dexcom Clarity via a compatible smart device: dexcom.com/compatibility. Healthcare providers will only be able to view a patient’s glucose data if the patient elects to share it with them through Dexcom Clarity. §§Comparison of NPS scores of Dexcom, Abbott, and Medtronic, Seagrove Survey 2021 Patient Perspectives. ##Libre 3 user guide
1 Dexcom, data on file, 2022. 2 Beck, RW, et al. JAMA. 2017;317(4):371-378. 3 Welsh JB, et al. J Diabetes Sci Technol. Jun 13 2022:19322968221099879. 4 Dexcom G7 CGM System User Guide. 2022. 5 Managed Markets Insights & Technology, LLC. MMIT Analytics, June 2022. 6 dQ&A US Q1 2021 Diabetes Connections Patient Panel Report. 2021;69-72. 7 IQVIA, February 2022. 8 Data on File. IQVIA 2022 9 Dexcom G7 User Guide. 10 GoodRx Program: Set buy down per finance of $200 for sensors and transmitters 11 American Diabetes Association. Standards of Medical Care in Diabetes - 2023. Diabetes Care. 2023;45(S1):S1-291. 12 Grunberger G, et al. Endocr Pract. 2021;27(6):505-537. 13 IQVIA, February 2022 - According to IQVIA, patient retention data is the sum of persistent and reinitiated patients. Persistent patients are the patients who remain on therapy without interruption (days’ supply + 30-day grace period). Reinitiated patients are the group that has interruption in use. These data are for new IIT patients across all channels from September 2020 to August 2021.
No. Dexcom G6 sensors, transmitters, and receivers are not compatible with the Dexcom G7 CGM app, sensors, nor receivers. If a compatible smart device is needed for the Dexcom G7 sensor, a patient must download the new Dexcom G7 app. The Dexcom G7 CGM system works with the existing Clarity and Follow apps.
Dexcom is working closely with its insulin pump partners to integrate Dexcom G7 into current and future automated insulin delivery systems as quickly as possible.
Calibration is not required but conducting optional blood glucose (BG) calibrations can move your patient’s sensor reading closer to their BG meter value.
The new Dexcom G7 CGM System requires sensors and a compatible display device. If your patient uses a compatible smart device, they will need to download the new Dexcom G7 app. An optional receiver is available as well.
Yes, Dexcom G7 is indicated for children as young as 2 years old.
Yes, Dexcom G7 CGM can be worn by pregnant patients with type 1, type 2 or gestational diabetes. CGM devices can be particularly beneficial for managing blood glucose levels during pregnancy, especially for those with diabetes or gestational diabetes. Dexcom G7 is for patients two years and older with any type of diabetes including type 1, type 2, or gestational diabetes.
Advantages of patients using a CGM system during pregnancy include:
• Closer monitoring of blood sugar levels: during pregnancy, glucose levels can fluctuate often, and continuous glucose monitoring can help patients make adjustments in real-time • Reduce risk of complications: Keeping patient glucose levels in target range can help reduce the risk of pregnancy complications.1,2
1 Yu F, et al. J Clin Endocrinol Metab. 2014.99(12).4674–4682. 2 Hapo Study Cooperative Research Group, Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008.358(19).1991-2002.
Yes, Dexcom G7 works with Dexcom Clarity.‡‡, Healthcare professionals and patients who used Dexcom Clarity with Dexcom G6 do not need to register again. The Dexcom G7 app and receiver also conveniently integrates a Dexcom Clarity data summary for quick and easy insights.
Pricing will vary depending on insurance coverage. Dexcom has been the #1 covered CGM brand,5 and our goal is to reach equal insurance coverage for Dexcom G7 as soon as possible. Dexcom will also have a quick start program allowing commercially insured patients to receive special pricing until their health plan covers it.
Dexcom G7 is for patients two years and older with any type of diabetes including type 1, type 2, or gestational diabetes.
| New features with Dexcom G7: | Dexcom G6 features included with Dexcom G7: |
|---|---|
|
|
§Fingersticks required for diabetes treatment decisions if symptoms or expectations do not match readings.
¶¶ Medicare coverage requires use of receiver
*Smart device, sold separately, required to display readings on watch. †Compatible smart devices sold separately. For a list of compatible devices, visit dexcom.com/compatibility. ‡Dexcom G7 can complete warmup within 30 minutes, whereas other CGM brands require up to an hour or longer. ||Results obtained with a prior generation Dexcom CGM System. ¶Separate Follow app and internet connection required. Users should always confirm readings on the Dexcom G6 app or receiver before making treatment decisions. #Compared to a prior generation Dexcom CGM System. **Dexcom G7 can complete warmup within 30 minutes, whereas other CGM brands require up to an hour or longer. ††Healthcare providers can register for Dexcom Clarity at clarity.dexcom.com/professional/ registration. ‡‡An internet connection is required for patients to send their glucose data to Dexcom Clarity via a compatible smart device: dexcom.com/compatibility. Healthcare providers will only be able to view a patient’s glucose data if the patient elects to share it with them through Dexcom Clarity. §§Comparison of NPS scores of Dexcom, Abbott, and Medtronic, Seagrove Survey 2021 Patient Perspectives.
1 Dexcom, data on file, 2022. 2 Beck, RW, et al. JAMA. 2017;317(4):371-378. 3 Welsh JB, et al. J Diabetes Sci Technol. Jun 13 2022:19322968221099879. 4 Dexcom G7 CGM System User Guide. 2022. 5 Managed Markets Insights & Technology, LLC. MMIT Analytics, June 2022. 6 dQ&A US Q1 2021 Diabetes Connections Patient Panel Report. 2021;69-72.
Dexcom G7 offers a better way to help your patients gain greater control of their diabetes, so they can more confidently manage it each day. Its low-profile, all-in-one wearable sensor warms up faster than any other CGM on the market,‡ sending real-time glucose readings automatically to a compatible smart device† or Dexcom receiver, no fingersticks§ required. Dexcom G7 also offers a suite of customizable alerts that can warn of high or low glucose levels and help you spend more time in range.||,2,3 Industry-leading remote monitoring and reporting capabilities also allow your patients to stay connected with their loved ones and your care teams anytime, anywhere.¶
§Fingersticks required for diabetes treatment decisions if symptoms or expectations do not match readings.
†Compatible smart devices sold separately. For a list of compatible devices, visit dexcom.com/compatibility. ‡Dexcom G7 can complete warmup within 30 minutes, whereas other CGM brands require up to an hour or longer. ||Results obtained with a prior generation Dexcom CGM System. ¶Separate Follow app and internet connection required. Users should always confirm readings on the Dexcom G6 app or receiver before making treatment decisions 2 Beck, RW, et al. JAMA. 2017;317(4):371-378. 3 Welsh JB, et al. J Diabetes Sci Technol. Jun 13 2022:19322968221099879.
Dexcom sensors are manufactured with a special adhesive to help them stick to patients’ skin after sensor insertion. Adhesive supplements may also be used.
- Liquid adhesive agents can be used with the sensor adhesive patch.1,2 A suggestion for patients when using liquid adhesive agents is to:
1. Create an empty oval on the skin with the liquid adhesive product.
2. Let skin adhesive dry.
3. Insert sensor on clean skin in center of oval.
- Additional adhesive patches or tape can be applied over the sensor adhesive patch.1,2 Suggestions for patients when using adhesive patches or tapes are to:
- Cut a hole in the adhesive patch or tape to fit around transmitter.
- Cut the adhesive patch or tape into strips to use ‘‘picture frame’’ technique around sensor adhesive patch.1,3
For detailed step-by-step instructions on how to use the Dexcom G6 Continuous Glucose Monitoring (CGM) System, please refer to the user guide. Dexcom, Inc. does not recommend, endorse or warrant any third-party products, including adhesive supplements and removal products.
View the downloadable "What Works for Me" document, which outlines the step-by-step process for how to insert and remove a Dexcom G6 sensor patch.
1. Chase HP, Messer L: Understanding Insulin Pumps and Continuous Glucose Monitors. 3rd ed. Denver: Children’s Diabetes Research Foundation, 2016.
2. Englert K, Ruedy K, Coffey J, et al.: Skin and adhesive issues with continuous glucose monitors: a sticky situation. J Diabetes Sci Technol 2014;8:745–751.
3. Ives B, Sikes K, Urban A, et al.: Practical aspects of realtime continuous glucose monitors: the experience of the Yale Children’s Diabetes Program. Diabetes Educ 2010;36: 53–62.
If patients experience difficulty removing the sensor from their skin, these products and techniques may help:
General Removal Techniques
- Loosen edge of adhesive with fingernail and use products listed below if necessary.1,2
- While removing tapes, use fingers of opposite hand to push skin down and away from adhesive. Continue to move fingers on skin toward adhesive as it is removed.2
- ‘‘Fold back’’ technique: Remove adhesive slowly, at low angle, folding back on itself.2
- ‘‘Stretch and relax’’ technique: Films that stretch (e.g., IV3000 or Tegaderm) may be stretched horizontally away from the center (opposite of the fold back technique) while walking fingers under the dressing to continue stretching it.2
- Use adhesive removal wipes to rub the skin under the tape toward the adhesive as it is removed. This helps loosen adhesive from skin and may help reduce pain with removal.1
Removal Products and Description
| Product | Description |
| Uni-solve Adhesive Remover (Smith&Nephew) | - Comes in wipes or liquid |
| AllKare Adhesive Removal Wipe (ConvaTec Inc) | - Comes in wipes |
| Tac Away Adhesive Removal Wipes (Torbot) | - Comes in wipes - Reciprocal product to Skin Tac |
| Detachol Adhesive Remover (Eloquest) | - Latex free, alcohol free - Comes in single use vials or liquid - Reciprocal product to Mastisol |
| Household oilsa: - Baby oil, coconut oil or olive oil |
- Least specialized and least expensive option |
For detailed step-by-step instructions on how to use the Dexcom G6 Continuous Glucose Monitoring (CGM) System, please refer to the user guide. Dexcom, Inc. does not recommend, endorse or warrant any third-party products, including adhesive supplements and removal products.
View the downloadable "What Works for Me" document, which outlines the step-by-step process for how to insert and remove a Dexcom G6 sensor patch.
1. Chase HP, Messer L: Understanding Insulin Pumps and Continuous Glucose Monitors. 3rd ed. Denver: Children’s Diabetes Research Foundation, 2016.
2. McNichol L, Lund C, Rosen T, Gray M: Medical adhesives and patient safety: State of the science: consensus statements for the assessment, prevention, and treatment of adhesive related skin injuries. J Wound Ostomy Continence Nurs 2013;40:365–380; quiz E361–E362.
a Used within institution or support in public commentary, online articles, diabetes blogs, social media.
Yes, Dexcom G6 is indicated for children as young as 2 years old.
Yes, Dexcom G6 does work with Clarity. Patients will not need to register again nor download a new Dexcom Clarity App if they have already established an account. If you are already sharing with your clinic, the clinic will not need to reconnect.
*To view a list of compatible smart devices, visit dexcom.com/compatibility.
‡This predictive alert can be triggered with impending hypoglycemia (glucose of 55 mg/dL or below is predicted to occur within the next 20 minutes).
§Based on the difference in A1C between baseline and measurements obtained 90 to 180 days thereafter.
||Prior to participating in any study procedures, each subject was asked to voluntarily document their consent by signing an Institutional Review Board (IRB) approved informed consent form.
¶Register for Dexcom Clarity at clarity.dexcom.com/professional/registration.
#An internet connection is required for patients to send their glucose data to Dexcom Clarity via a compatible smart device: dexcom.com/compatibility
**Healthcare providers will only be able to view a patient’s glucose data if the patient elects to share it with them through Dexcom Clarity.
††The reimbursement information provided is intended to assist you with billing for your services related to continuous glucose monitoring (CGM). It is intended for informational purposes only and is not a guarantee of coverage and payment. Providers are encouraged to contact their local payers with questions related to coverage, coding and payment. Rates provided under the Medicare PFS and OPPS are rounded to the nearest hundredth.
1 Puhr S, et al. Diabetes Technol Ther 2019;21(4):155-8.
2 Dixon, et al. Journal of Diabetes Science and Technology. 2020;14(5):908-911.
3 Grlben TR. Noar A Blalock 0, Polonsky WH. Chmge m Hemoglobin Ale and Quality of Life with Real-Time Continuous Glucose Momtonng Use by People with Insulin-Treated Diabetes in the Landmark Study. Diabetes Technol Ther 2021:23.S3S·S39
4 Champakanath A, et al. Diabetes Care. 2022;45(3):750-753.

