How is Dexcom CGM different from a blood glucose meter?
A glucometer measures the sugar levels in a patient's blood, while a Continuous Glucose Monitor (CGM) monitors the levels in interstitial fluid, the fluid between cells in your tissues. Traditional glucometers require a consistent supply of test strips for use, whereas Dexcom is an unblinded non-adjunctive CGM. The traditional method for patients of measuring glucose levels requires a fingerstick using a glucometer (blood glucose meter) which provides a glucose reading at a single point in time. The key difference between Dexcom CGM and a glucometer is that Dexcom CGM provides glucose readings throughout the day and night, including glucose speed and direction arrows that empower wearers with more information for more informed decision making•. Finally, Dexcom CGM is designed with alerts to warn the wearer of glucose highs and lows during critical times like playing, sleeping, or exercising to help wearers catch high and lows before they become critical. Here is an example of how Dexcom CGM information could impact glucose management decisions: Glucometer (BGM) READING: 119

CONTINUOUS GLUCOSE MONITOR (CGM) READING: 119
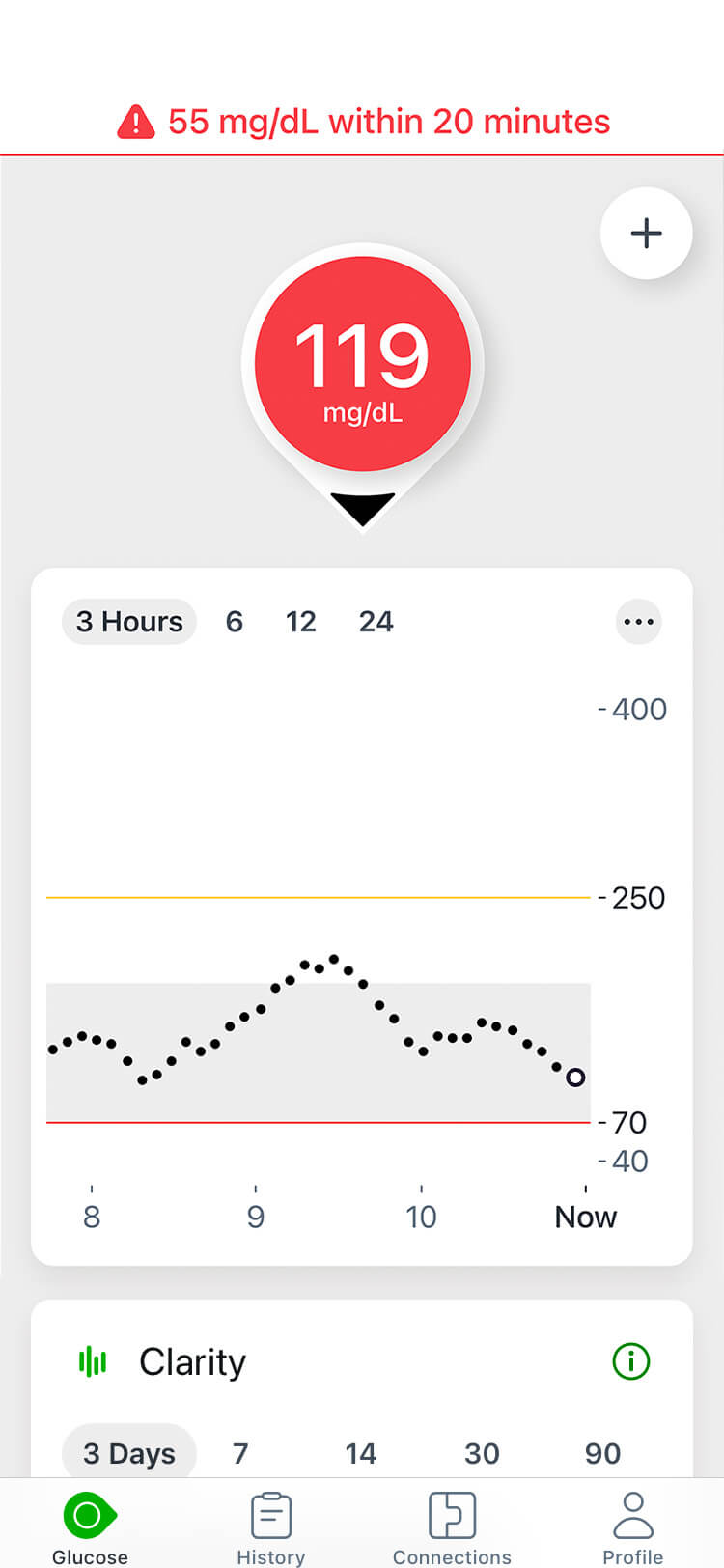
*smart devices sold separately.
(The straight down arrow signal a rapid decline in glucose)
Comparing cgm vs glucometer accuracy, both provided patients with current and accurate glucose readings. However, based on the Glucometer (BGM) reading of 119, this person is likely to decide that no action is required. But, with a similar glucose level reading on the Dexcom CGM and the straight down arrow, the patient might decide to eat some carbohydrates to avoid having a hypoglycemic event.



